With all the pain and suffering going on with people’s loved ones dying at the hands of corrupt healthcare systems and deadly protocols, you would think that everyone on this side of the fence would be banding together to take a common stand against a common enemy. At least, you would think. One group in particular doesn’t seem to feel this way and when another website or group sets out to help spread awareness, they take it upon themselves to spread vicious lies about the persons or groups who they think they are ‘in competition’ with them.
This group is Protocol Kills LLC. They’ve targeted several groups and their leaders and members, creating lies and a divide among the different groups sharing victim’s stories, including us, Fight For Christy Inc. Let’s dispel some of these rumors and lies and shed some light on the REAL Protocol Kills. The main members of their group are Greta Crawford, Therese Hernandez, Anthony Schenck, and Kristi Schmadl.
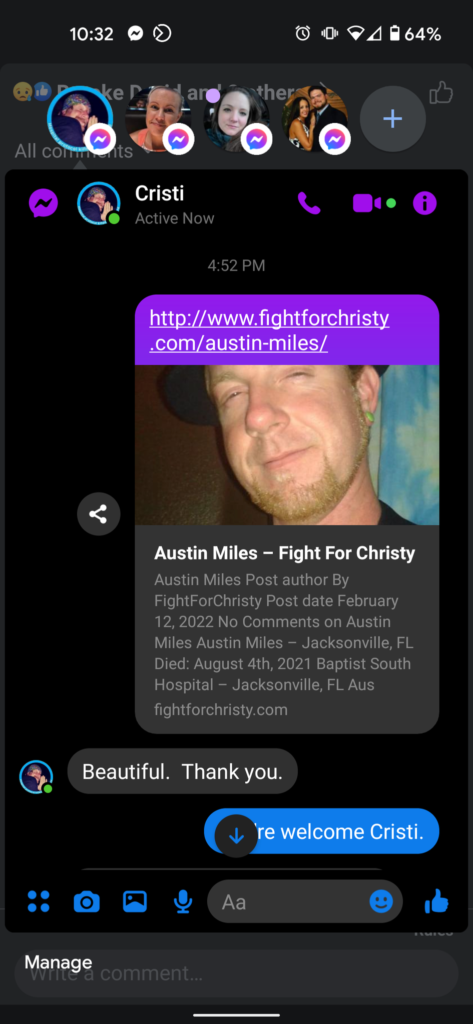
It all started back in February when we shared the story of Austin Miles, given to us by his wife, Cristi Miles. Cristi, like many others, shared his story with multiple sites, us included. We were given permission to post and share their story after Cristi was given the opportunity to read over what we were to share, as is what we do with every victim who shares their story with us. We shared it on Facebook including one of many Facebook groups dedicated to spreading awareness and sharing stories of our lost loved ones. Greta Crawford, who also goes by ‘Shannon Crawford’ in a secondary Facebook account, saw that we shared a story that was also on Protocol Kills and immediately went on the defensive and accused us of STEALING her work, begging for donations, searching out and contacting everyone they’ve posted stories about, and more. Let’s dive into these lies, shall we?
Stealing Stories
As we mentioned, this all started with Cristi and Austin’s story. You can ask anyone who’s story we have shared, we have a process. Those wanting to share fill out the story submission form and we ask them to provide some photos of their loved one. We don’t change the story, only correcting spelling and some formatting errors (converting 1 long paragraph into seperate paragraphs) while still maintaining the original content. Once we have completed the post, we then show it to them and gain their approval, and at that point and only that point do we share the story wherever we can. Images can be clicked for full resolution viewing.
This is pretty much our standard procedure. After creation, we allow the person who submitted a chance to review the content and offer up any requested changes. Until we get final consent, the story does not go any further.
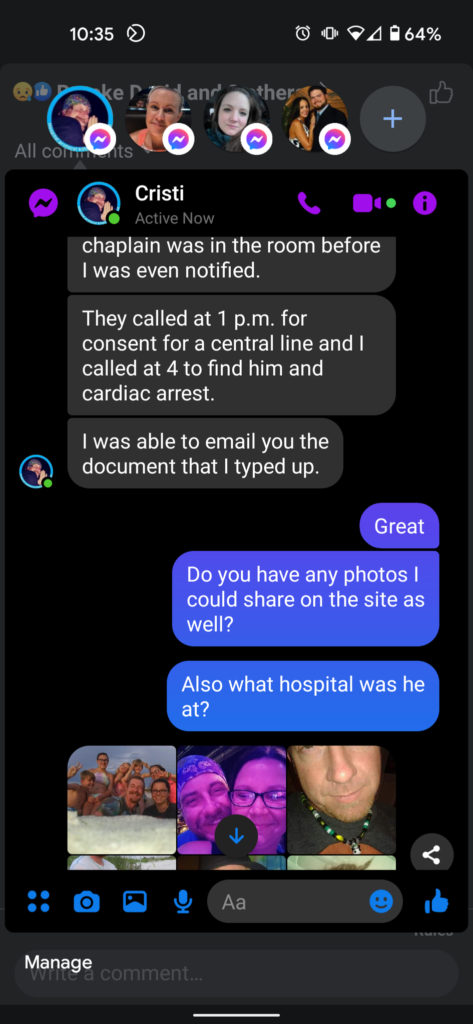
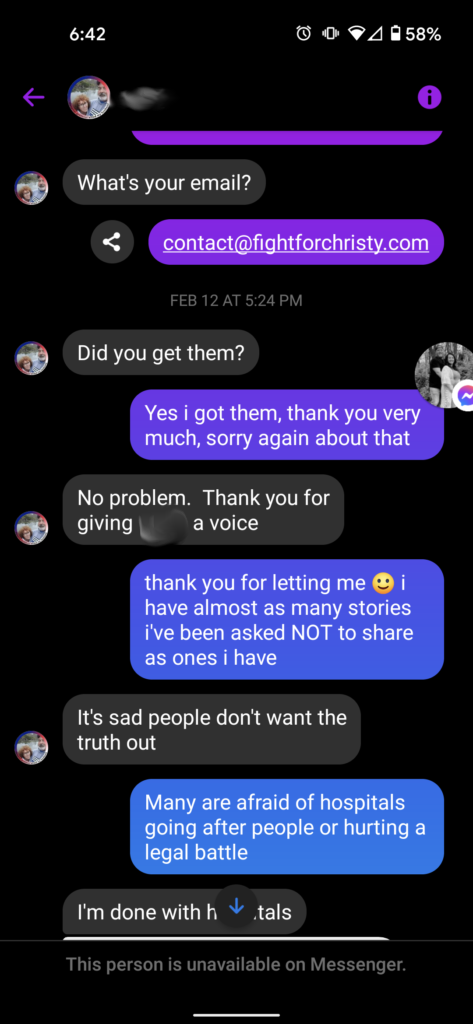
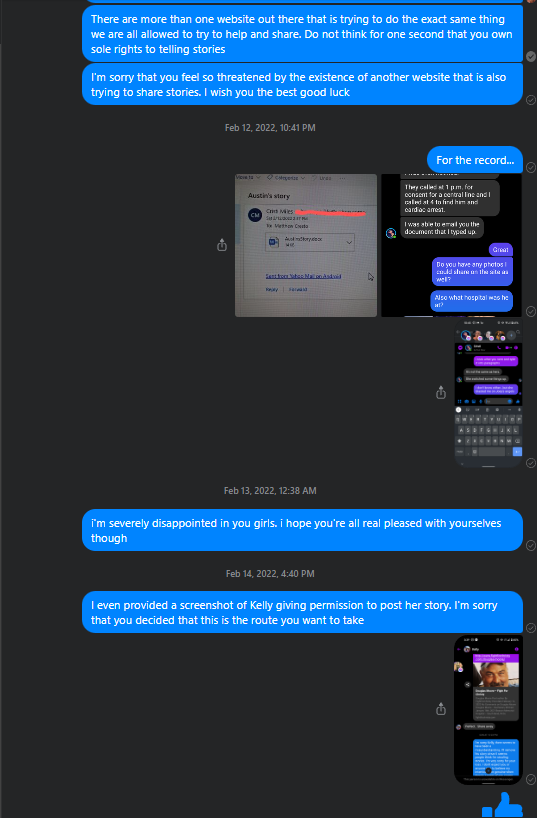
We don’t create our own content. We only use what’s supplied to us. Here you see Cristi say that she was able to email us the document (story) we requested, as well as sending us photos to use
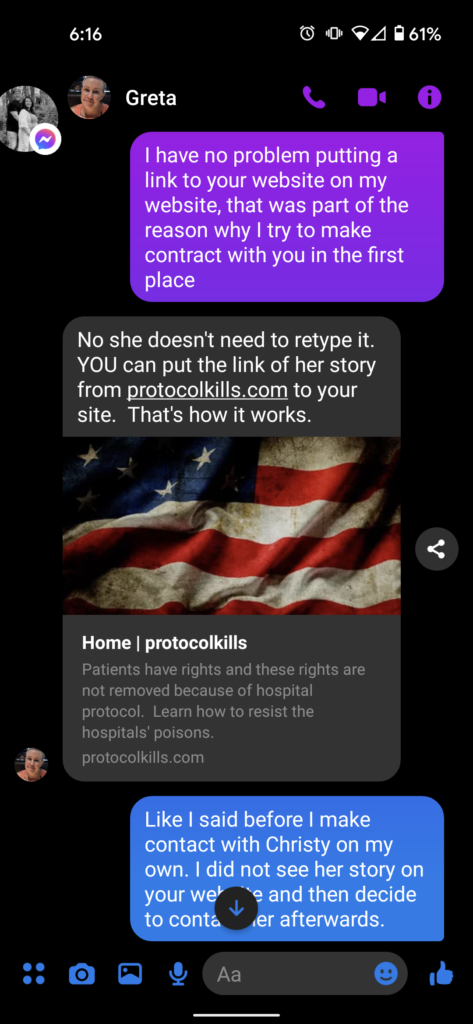
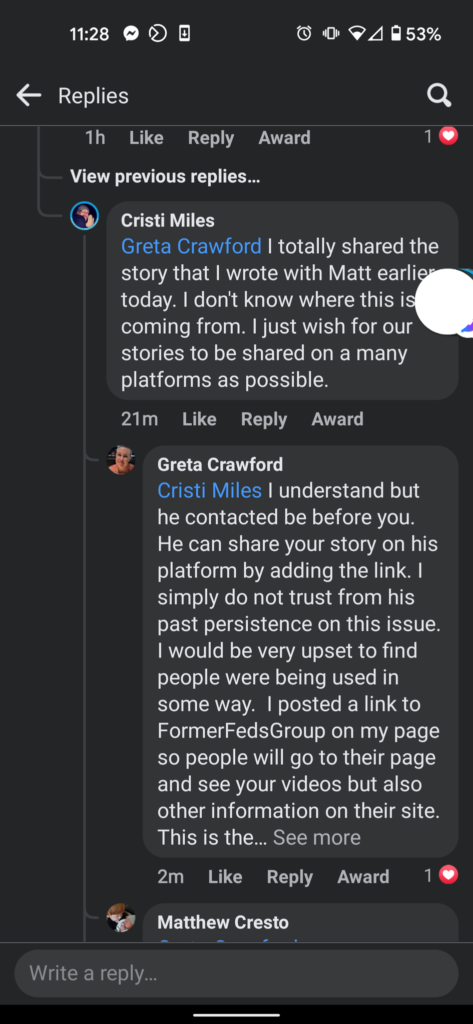
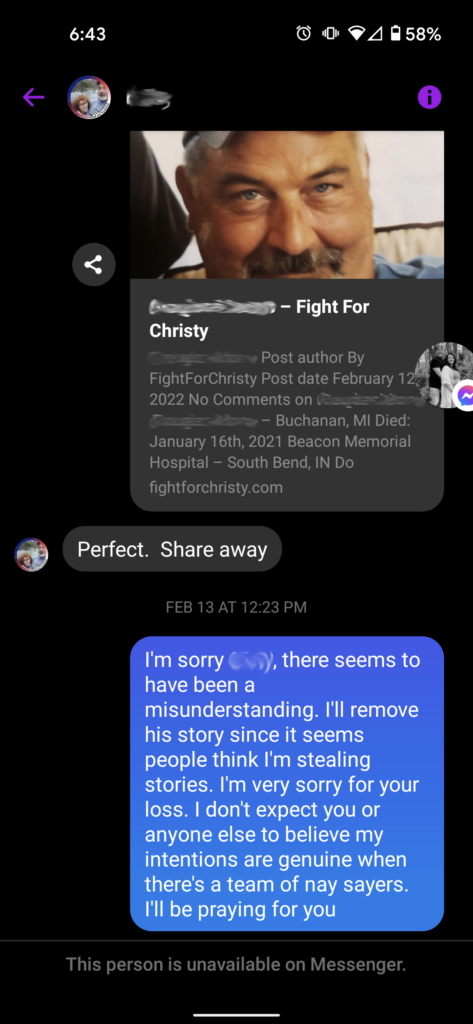
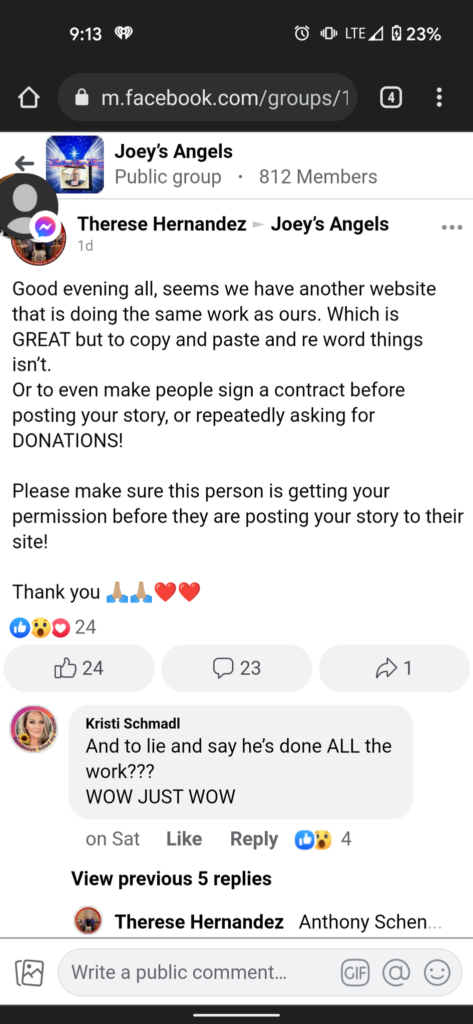
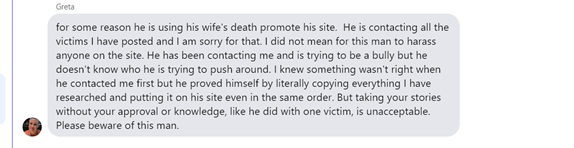
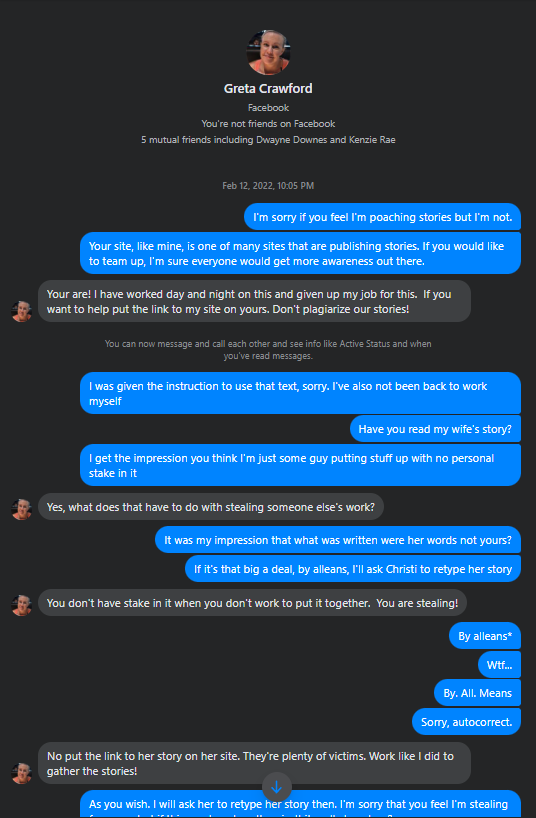
We figured this would be enough proof to Greta that we didn’t steal anything from her, but apparently it was not. Greta commented on one of the posts we made in a group, and Cristi even came to our defense! That didn’t matter to Greta, she wants to be the ONLY place to read these stories, as she demands multiple times that we delete the story and instead post a link to the story that she posted on her site!
Greta even managed to instill enough fear into one of the people who shared a story with both of us, that they felt the need to lie and go along with whatever Greta said, also accusing us of stealing her story and posting it without permission. She reportedly told Greta and Therese that she asked us multiple times to delete the story and that we never had permission to post it in the first place. Had she actually asked us to remove it, we would have done so immediately. While going through the process of creating the post for her, she spoke of how “It’s sad people don’t want the truth out”. Pot…..meet Kettle.
To date, we still have yet to see Greta produce any evidence of any of her claims.
Begging for Donations / Making money off victims
As if being accused of stealing stories isn’t bad enough, Greta and Therese have publicly claimed multiple times that I (Matthew Cresto) am keeping the donation money we receive for personal use. I offered up all bank records and paypal records to show this just isn’t the case, but they continue to tell people these same lies.
So apparently we are making money off of donations. Again… Pot, meet Kettle. Maybe Greta just feels guilty for taking advantage of people? Here’s her February 17th newsletter…
Taking donations and selling low quality shirts at high prices, for what? To pay your personal bills? Sounds a lot like what you accused us and others of.
Greta, my offer still stands. Let’s compare bank and paypal statements!
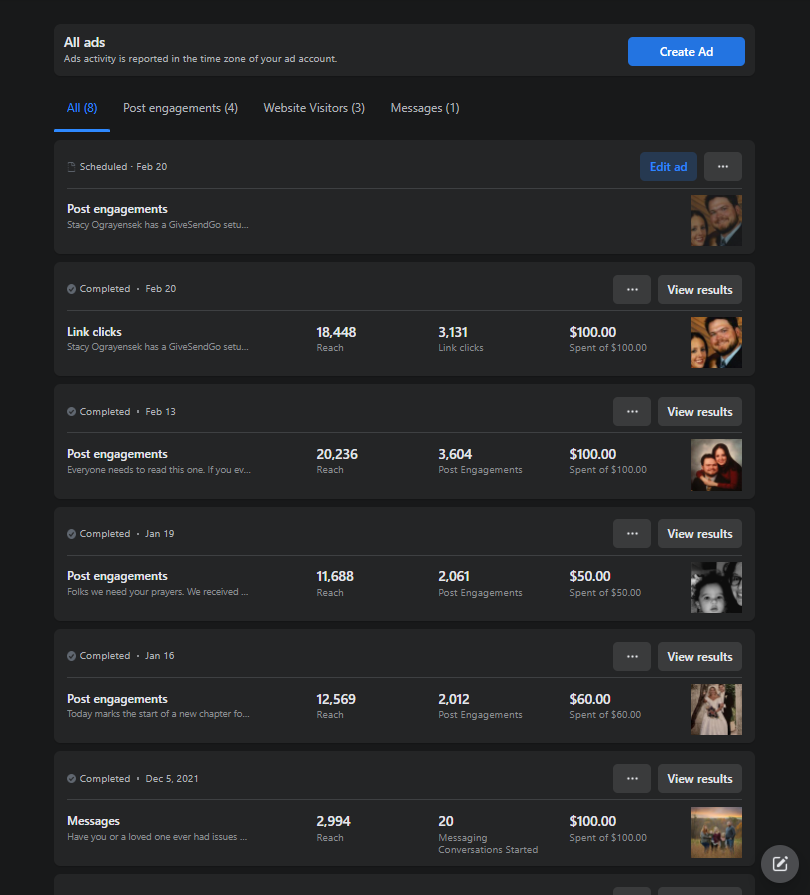
All of our donations are only used towards helping others. Not 1 penny (including my initial investment in the business) ever goes to myself or anyone I’m related to. One of the things we do is pay for Facebook advertising for our posts and some of the stories we’ve shared. Examples :
We pay for spreading the word…What’s Greta do?
Searching out everyone they’ve shared
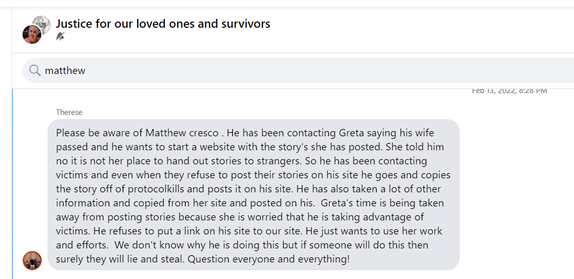
It’s no secret, traffic doesn’t just come to you automatically. You have to do the leg work and find people willing to tell their stories. What’s not true is the methods Greta and Therese insist we’ve been using. Yes we’ve contacted people on Facebook in several groups, looking for signs of loss, such as saying “my <insert relative> died of <insert cause>” but we’ve never directly gone to any website sharing stories to hunt them down on Facebook. Protocol Kills however has done something like this! One of the other websites targeted by them has a support group meeting, similar to a Zoom call. Therese requested that Anthony be invited to the support group meeting and he was. Little did this group know it was a trap. Anthony began making comments about ‘taking money from victims’ (hmm sounds familiar?) and amazingly, after the meeting was over, all of the people who had joined began receiving emails from Protocol Kills asking for them to share their story with Protocol Kills.
To be completely transparent, once we started sharing the stories of others, WE DID reach out to Protocol Kills with the intent of bringing LOTS of websites together to collaborate and share stories, studies, etc. Instead of replying they weren’t interested they just ignored my email. At no time did I say I’d give them Christy’s story in exchange for any number of their stories, let alone an exact number of 54 Therese is claiming above.
Real classy guys. So again it seems Protocol Kills is doing EXACTLY what they accuse others of doing…even to groups THAT SUPPORTED THEM.
Threats
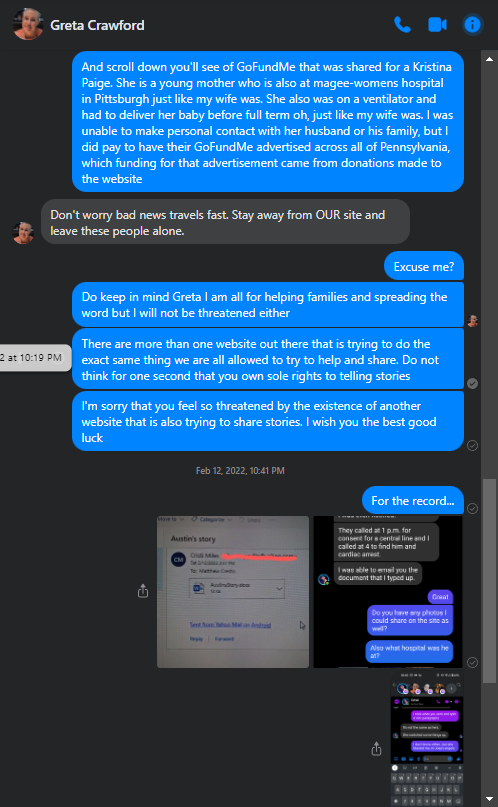
Greta says we’ve threatened her. In what way? Yes we did warn them that unless they removed the blatant lies to defame and discredit myself and our work, I may take legal action. Claims of harassment, bullying, stalking, and threats should not be taken lightly, yet Greta has no problem with making them herself.
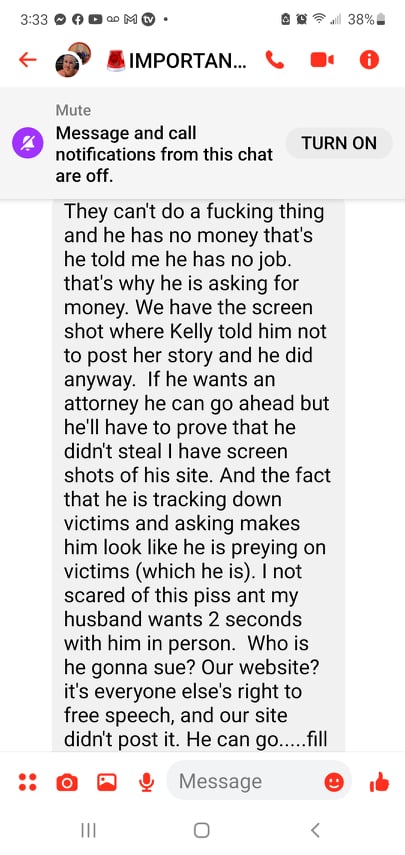
2 second in person? What are we going to do Greta? Hold hands and sing Kumbaya? This was a screenshot sent to me by Anthony Schenck just before he ended the conversation.
I’m starting to see a pattern here…EVERYTHING they accuse us and others of, is exactly what they’re doing themselves.
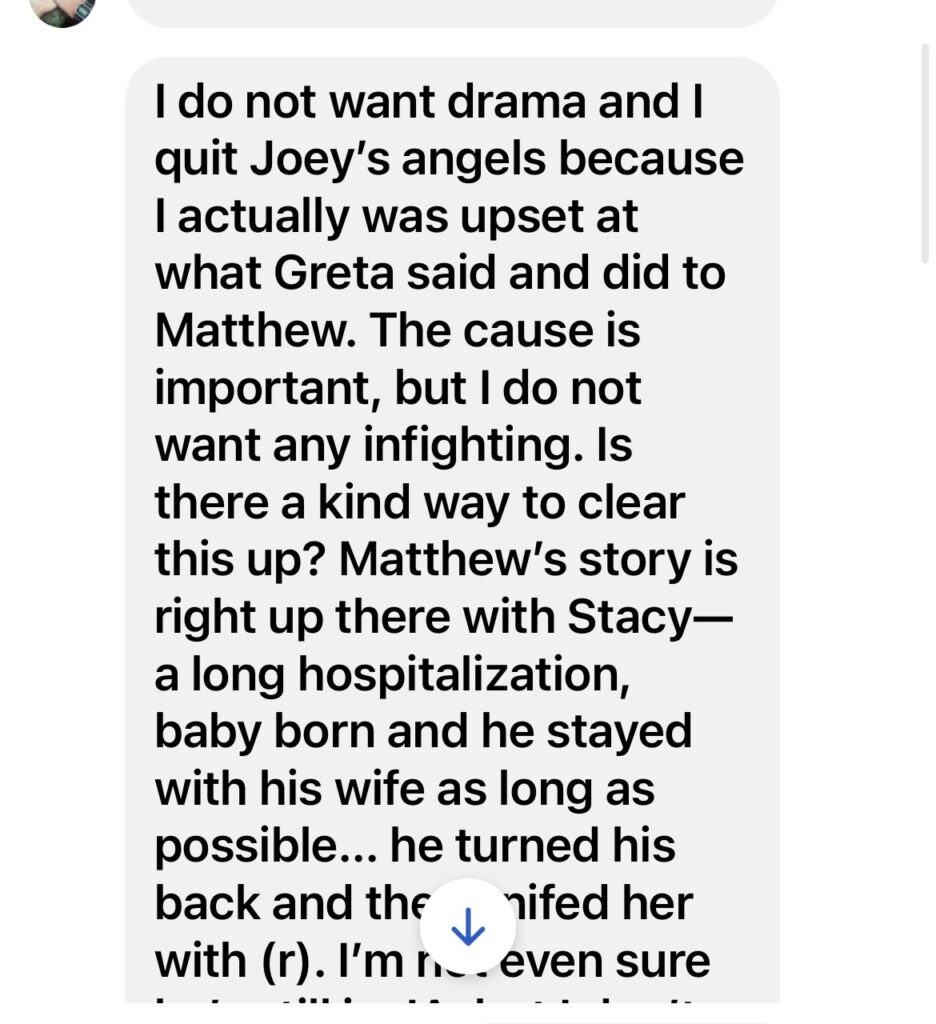
Greta’s actions and posts have caused a division in a movement that was supposed to bring everyone together for a common cause. Instead, she makes victims feel like they have to stay quiet or they’ll be punished too.
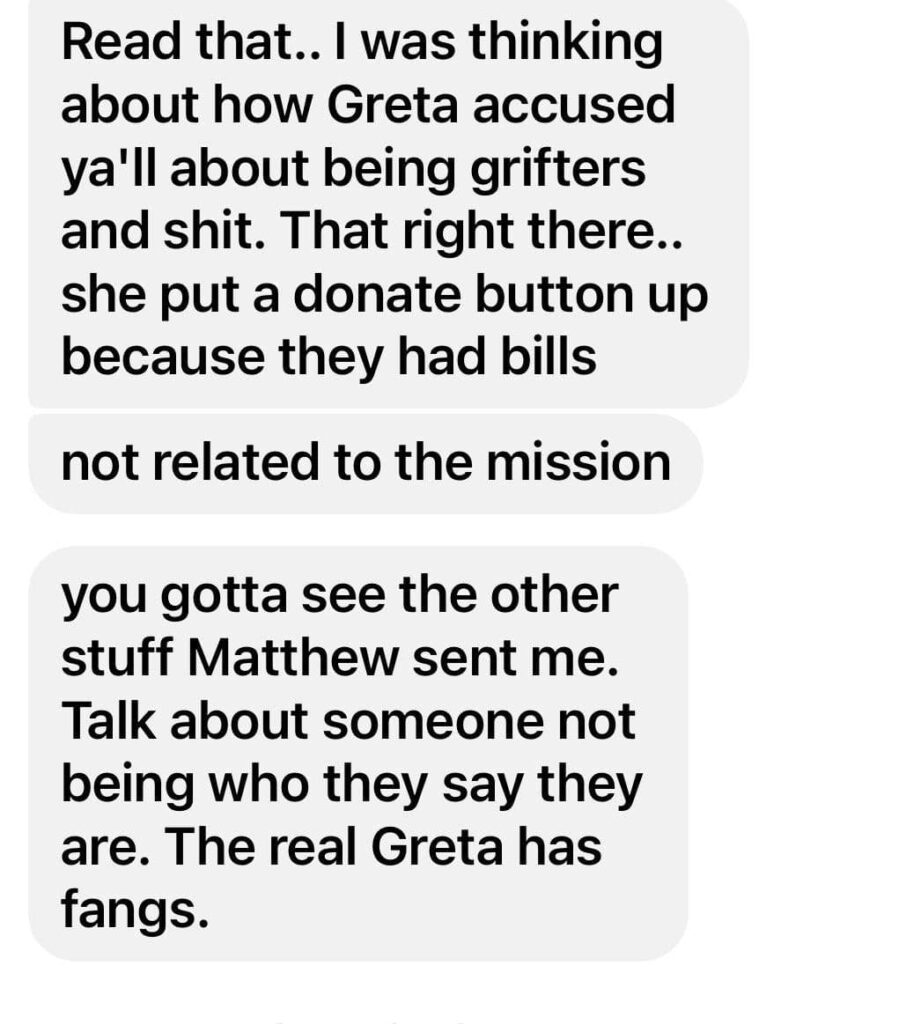
These were sent in anonymously:
Safe to say, a lot of wrong has been done. This is my account of it, and I promised transparency. Believe what you will, but do be careful about what source you want to believe, because they may be lying to you.
Oh while we’re on the topic of dishonesty! We mentioned Anthony Schenck a while ago. Guess what we found out about Mr. Schenck? The interesting stuff starts on page 5…
Yep. Marijuana, Methamphetamines, Assult, Fraud, Unauthorized use of a vehicle …and this convicted felon represents Protocol Kills?
Hypocrisy
This is a lovely recent post that Greta made… How many times can the pot call the kettle black?
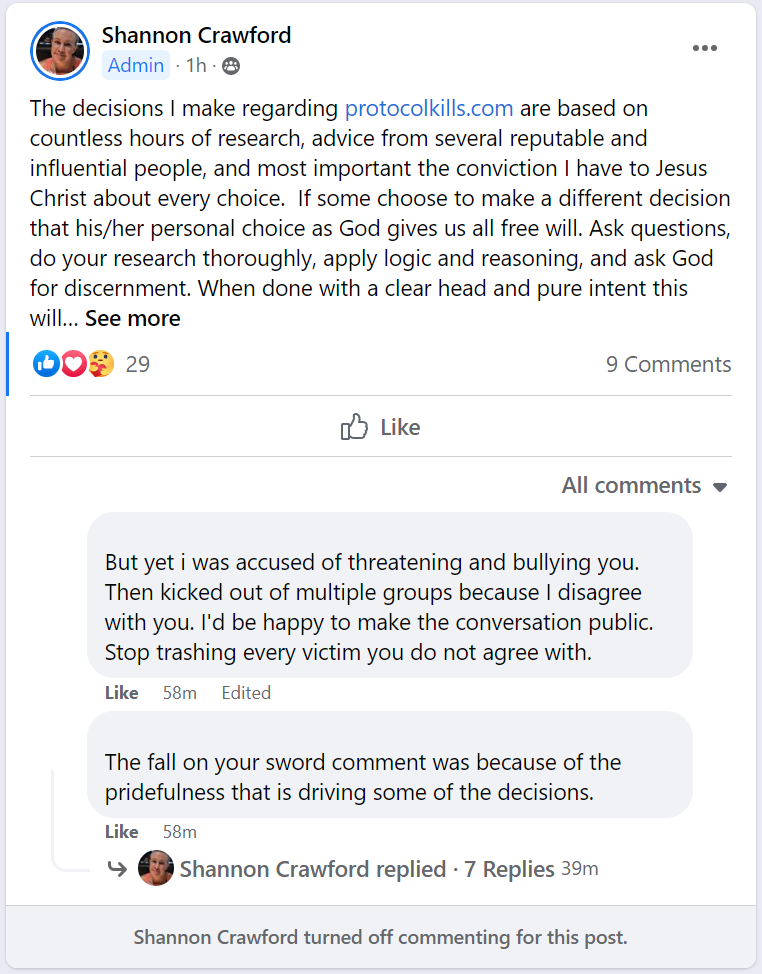
Transparency
Here’s the full chat with Greta. Make your own conclusions. Please click on image to expand.
Conclusion
I know of at least 3 groups that she has ruined a relationship with and spread lies about, and at least 20 people that have come forward about what Greta is really like.
It’s not my intent to persuade anyone’s way of thinking one way or another. The damage has already been done and nothing can change that. You’re all free to make your own judgements. This is just my honest account of everything that’s happened. Knowledge is power, and Truth above all is most important, not ratings, not how many followers you have, not how many social media posts you make, but being true to yourself and being honest with others.